About Us
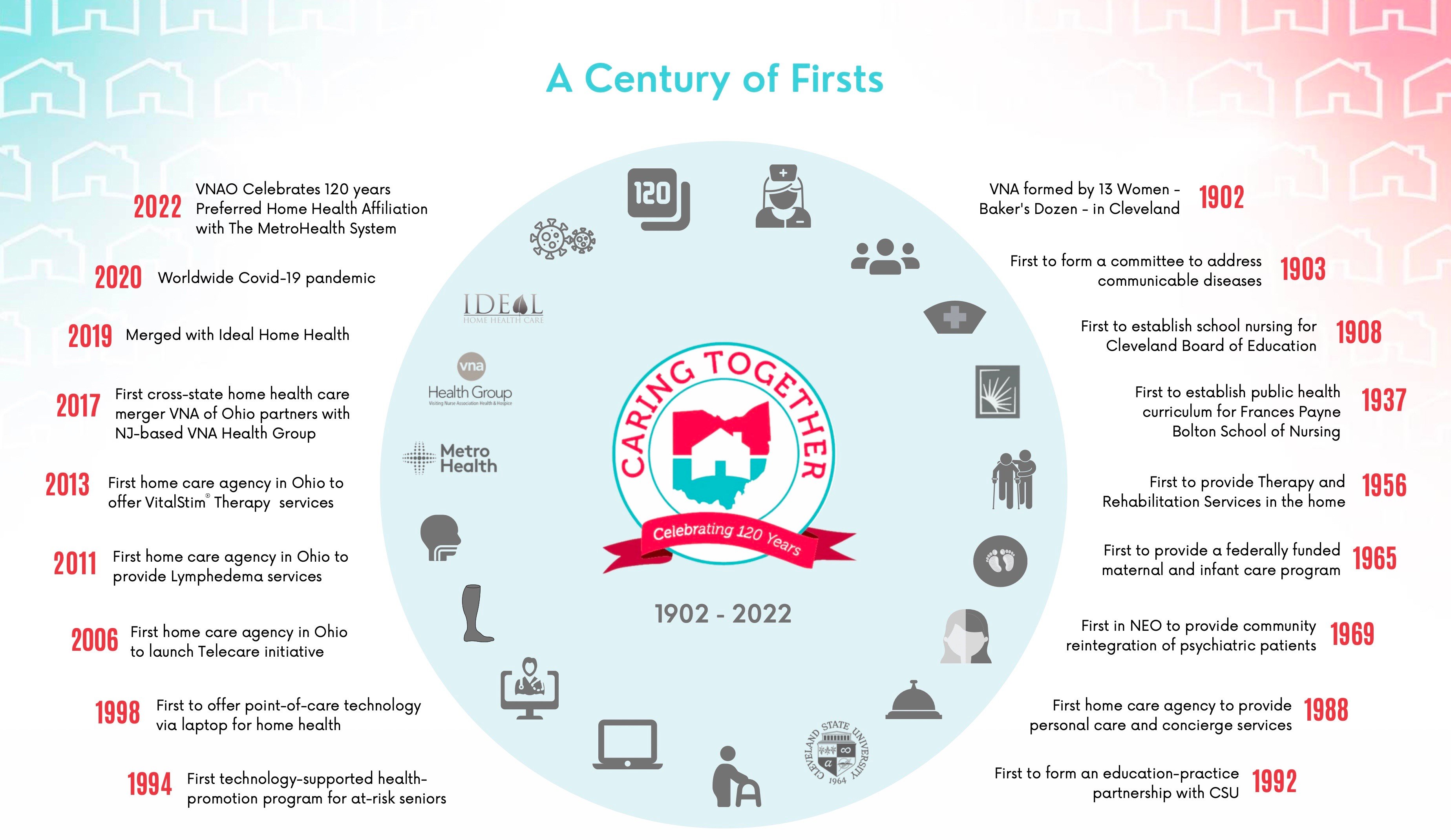
Our Legacy: A Century of Firsts
In 1902, 13 pioneering women created the Visiting Nurse Association of Cleveland, now VNA of Ohio, and set out to meet the health care needs of their community.
Today, we celebrate over 120 years of service. Our not-for-profit organization has grown as VNA of Ohio and serves thousands of patients and clients across the Northeast and Mid-Ohio region.
We offer the largest scope of home-based services throughout 9 Ohio counties. In 2017, VNA of Ohio joined New Jersey-based Visiting Nurse Association Health Group to better serve Ohio with more high-quality and innovative home-based care services.
As our history shows, VNA of Ohio is responsive to our community's needs because it is our mission, it is at our core. Your care is our focus.
As a leader and the first to serve and strengthen healthcare within our community, our strong legacy will continue to grow.
Your Care is Our Focus.
The entire VNA of Ohio health care team works diligently to fulfill our mission. We offer patients and clients high-quality, comprehensive care that promotes the independence and dignity of those we serve and aim to serve our entire community, regardless of their material circumstance.
Our home-based health care services place your needs first.
Our mission
To provide high quality, comprehensive home health and hospice care to promote the independence and dignity of those living in the communities we serve.
Our values
- We provide holistic, compassionate, and accommodating care of patients and clients regardless of their financial circumstances
- We invest in research and development of cutting edge, technologically superior, community need inspired physical and mental health programs
- We believe in a team philosophy and offer opportunities for growth in our leadership, medical and business staff, and volunteers


Our accreditations, certifications, and memberships
- Medicare and Medicaid Certified Agency
- CHAP Certified
- Ohio Department of Health
- Licensed Community Mental Health Agency
- United Way Agency
- Ohio Council for Home Care and Hospice
- National Association of Homecare and Hospice
- Leading Age Ohio
VNA of Ohio Provides Many Types of Home Healthcare Services.
How Can We Care for You Today?
Home Health Care
- Medication management
- Recovery from injury or illness
- Chronic disease management
- Infusion therapy
- Wound and ostomy management
- Cardiac monitoring
- Home health aide
Medical Surgical Nursing
- Primary care
- Palliative care
- Transitional care
Hospice
- Ongoing medical care and coordination
- Crisis support 24/7
- Expert pain and symptom management
- Patient, caregiver education and companion support
Mental & Behavioral Health
- C.A.R.E program for Mental and Behavioral Health
- Anxiety and depression disorders
- Safe shelter, nutrition, and medication plans
Private Duty
- Assistance with walking and transferring
- Assistance with exercises
- Personal care and grooming
- Meal planning
Rehabilitation
- Ongoing medical care and coordination
- Crisis support 24/7
- Expert pain and symptom management
- Patient, caregiver education and companion support
VNA of Ohio Home Health Care is licensed in OH and accredited by CHAP. We are Medicare and Medicaid certified and our skilled services are covered by the patient's health care insurance benefit.

Our patients and clients experience our amazing care every day.
"Our nurse, Jessica, was very polite, funny, personable, showed great care and concern and it felt like she was a part of the family. While taking care of my wife, I felt she stood out above the rest and is a special nurse. We need more people like her!"
